Understanding Corneal Transplant
A corneal transplant is a surgical procedure that replaces a damaged or diseased cornea with healthy donor tissue. The cornea is the clear, dome-shaped surface at the front of the eye that focuses light and plays a critical role in vision. When the cornea becomes cloudy, scarred, or distorted, it can severely impact eyesight, making daily activities challenging. Corneal transplants are performed to restore vision, relieve pain, and improve the appearance of the eye. There are several types of corneal transplants, each suited for specific eye conditions. Penetrating Keratoplasty involves replacing the full thickness of the cornea. Endothelial Keratoplasty focuses on replacing only the inner layer of the cornea, while Deep Anterior Lamellar Keratoplasty targets the outer layers, preserving healthy tissue. Understanding the different approaches helps patients and families make informed decisions about treatment options.
Who Needs a Corneal Transplant
Corneal transplants are recommended for individuals whose corneal damage cannot be corrected with glasses, contact lenses, or less invasive procedures. Common conditions that lead to the need for a transplant include keratoconus, where the cornea thins and bulges into a cone shape, and Fuchs’ dystrophy, a degenerative condition affecting the cornea’s inner layer. Severe infections, corneal ulcers, and traumatic injuries can also necessitate a transplant. Risk factors that may require surgical intervention include prolonged eye inflammation, previous eye surgeries, and genetic conditions affecting corneal health. Patients often experience symptoms such as blurred vision, glare, halos around lights, and eye discomfort before surgery becomes necessary. Early evaluation by an ophthalmologist can help identify the severity of the corneal issue and determine whether a transplant is the best course of action. Recognizing these warning signs ensures timely intervention and better outcomes.
Preparing for Corneal Transplant Surgery
Preparation for corneal transplant surgery begins with a comprehensive eye examination. Eye specialists evaluate visual acuity, corneal thickness, and overall eye health. Pre-surgery diagnostic tests often include corneal topography, pachymetry, and endothelial cell count to assess suitability for the procedure. Patients may be advised to adjust medications, manage systemic conditions such as diabetes, and discontinue certain eye drops before surgery. Lifestyle considerations, including avoiding smoking and maintaining a healthy diet, can contribute to faster healing. On the day of surgery, patients receive instructions about fasting, anesthesia, and post-surgery care. Being well-prepared helps reduce anxiety and ensures that the procedure proceeds smoothly.
The Corneal Transplant Procedure
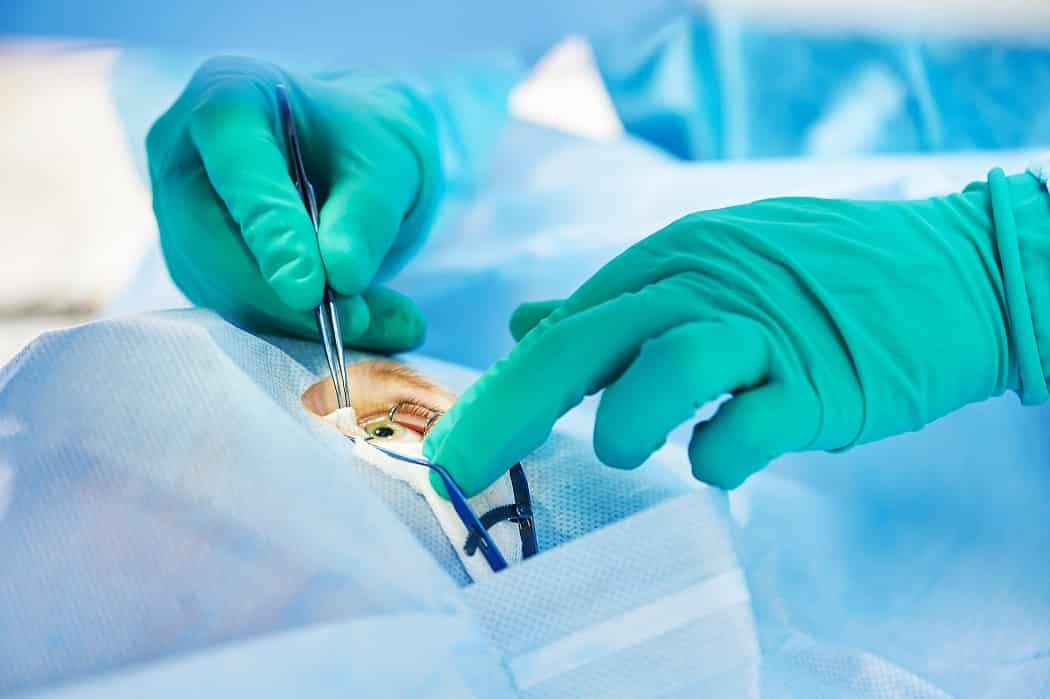
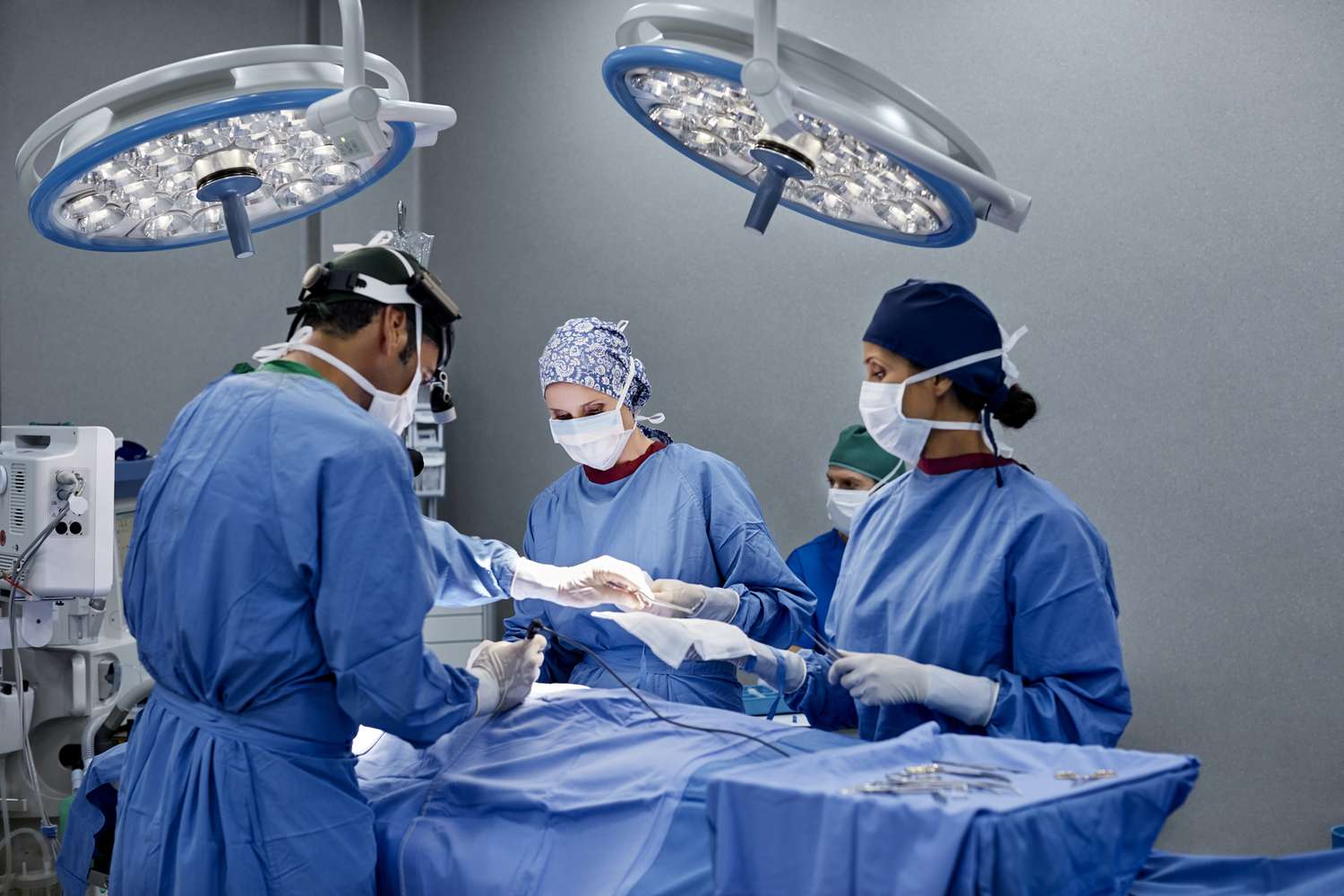
The corneal transplant procedure involves replacing damaged corneal tissue with a healthy donor cornea. Donor tissue is carefully matched to the recipient’s eye to reduce the risk of rejection. The surgical process begins with numbing the eye using local or general anesthesia, depending on the patient’s condition. Surgeons use precision instruments to remove the diseased portion of the cornea and replace it with the donor tissue. The graft is then secured with fine stitches or special adhesives that promote healing. Surgery typically lasts between one to two hours, though the exact duration depends on the type and complexity of the transplant. Patients usually experience minimal discomfort during the procedure, and advances in surgical techniques have significantly improved safety and outcomes.
Recovery and Rehabilitation
Recovery after a corneal transplant is a gradual process requiring patience and careful care. In the first few days, patients may experience mild discomfort, light sensitivity, and blurred vision. Eye drops and medications are prescribed to prevent infection and reduce the risk of rejection. Activity restrictions, such as avoiding heavy lifting, swimming, or rubbing the eyes, are essential to protect the new cornea. Follow-up visits with the ophthalmologist are scheduled to monitor healing and detect early signs of complications. Over weeks and months, vision gradually improves, though it may take up to a year for full visual clarity. Rehabilitation may include corrective lenses or minor procedures to optimize vision. Consistent adherence to post-surgery instructions significantly increases the likelihood of a successful outcome.
Risks, Complications, and How They Are Managed
While corneal transplants are generally safe, they carry some risks that patients should understand. Possible complications include graft rejection, infection, elevated eye pressure, and astigmatism. Signs of rejection may include redness, pain, light sensitivity, and decreased vision, which require prompt medical attention. Preventive strategies include proper use of prescribed medications, routine eye checkups, and protecting the eye from trauma or infection. Some patients may require additional procedures or interventions to address complications. Long-term monitoring ensures the transplanted cornea maintains clarity and functionality. Awareness of potential risks and early intervention can significantly improve outcomes and safeguard eye health.
Advancements in Corneal Transplantation
Modern corneal transplant techniques have evolved to improve safety, precision, and recovery time. Minimally invasive procedures, such as endothelial keratoplasty, allow surgeons to replace only the affected layers, preserving healthy tissue and reducing healing time. Artificial corneas and tissue engineering are emerging options for patients with limited donor tissue availability. Advanced imaging and surgical tools enable more accurate graft placement and lower complication rates. Researchers are exploring regenerative medicine approaches to stimulate corneal cell growth and reduce dependence on donor tissue. These advancements are making corneal transplants more accessible and effective for a wider range of patients. Staying informed about new techniques can help patients discuss the best options with their ophthalmologist.
Living with a Corneal Transplant
After a corneal transplant, many patients experience significant improvement in vision, though full recovery requires time and care. Adjusting to new vision may involve learning how to manage light sensitivity and depth perception changes. Patients are encouraged to maintain regular follow-ups, use prescribed eye drops consistently, and protect their eyes from injury. Emotional and psychological support can be crucial, as vision restoration often impacts quality of life and confidence. Lifestyle adjustments, including limiting screen time and practicing eye hygiene, contribute to long-term success. Joining support groups or connecting with others who have undergone corneal transplants can provide guidance and encouragement. Embracing these practices helps ensure the best possible outcome for vision and overall eye health.
Frequently Asked Questions (FAQ)
- How long does a corneal transplant last?
Most corneal transplants can last 10 to 20 years, though longevity depends on the patient’s overall eye health and adherence to post-surgery care. - Is corneal transplant painful?
Discomfort is typically mild and manageable with prescribed medications. Modern anesthesia minimizes pain during surgery. - How soon can I see clearly after surgery?
Vision gradually improves over weeks to months, with optimal clarity often achieved within a year. - Can a corneal transplant be repeated?
Yes, if graft failure or rejection occurs, another corneal transplant may be performed. - What are the chances of rejection, and how is it treated?
Graft rejection occurs in a small percentage of cases. Prompt treatment with medications such as corticosteroids can often reverse it. - Are there alternatives to corneal transplants?
Alternatives include specialized contact lenses, corneal cross-linking for keratoconus, and emerging artificial cornea implants.
Takeaway
Corneal transplant surgery offers life-changing improvements in vision and eye health for individuals with damaged or diseased corneas. Understanding the procedure, preparation, recovery, and potential risks empowers patients to make informed decisions. Advances in surgical techniques and technology continue to enhance outcomes and reduce recovery time. By following medical guidance and adopting healthy practices, patients can enjoy improved vision and quality of life. For anyone experiencing significant corneal damage or vision impairment, consulting an ophthalmologist about corneal transplant options is a crucial step toward restoring clarity and comfort in everyday life.