Understanding Decubitus Ulcers
Decubitus ulcers, commonly referred to as pressure ulcers or bedsores, are injuries to the skin and underlying tissue caused by prolonged pressure on specific areas of the body. These ulcers often develop in individuals who have limited mobility, such as those confined to a bed or wheelchair for extended periods. The constant pressure reduces blood flow to the skin, depriving tissues of oxygen and nutrients, which eventually leads to tissue breakdown. Common areas where these ulcers appear include the heels, hips, tailbone, and elbows because these regions bear the most weight when a person remains in one position. The condition can begin subtly, often with skin discoloration or mild discomfort, but can progress rapidly if not addressed early. Understanding how these ulcers form is essential in guiding effective decubitus ulcer treatment strategies. Early awareness empowers caregivers and patients to act promptly, preventing minor skin issues from escalating into severe wounds.
Causes and Risk Factors Behind Pressure Ulcers
Several factors contribute to the development of pressure ulcers, and understanding these causes is essential for effective prevention and treatment. One of the primary causes is prolonged immobility, which restricts blood flow and increases pressure on certain body parts. Friction and shear forces also play a significant role, especially when the skin rubs against bedding or clothing, causing irritation and damage. Moisture from sweat, urine, or feces can weaken the skin’s protective barrier, making it more susceptible to injury. Certain medical conditions such as diabetes, vascular diseases, and malnutrition further increase the risk by impairing the body’s ability to heal. Elderly individuals are particularly vulnerable due to thinner skin and reduced elasticity. Wheelchair users and bedridden patients are also at higher risk because of continuous pressure on limited areas. Recognizing these factors is a critical step in developing a targeted decubitus ulcer treatment plan that addresses both the root causes and symptoms.
Stages of Decubitus Ulcers and Their Severity
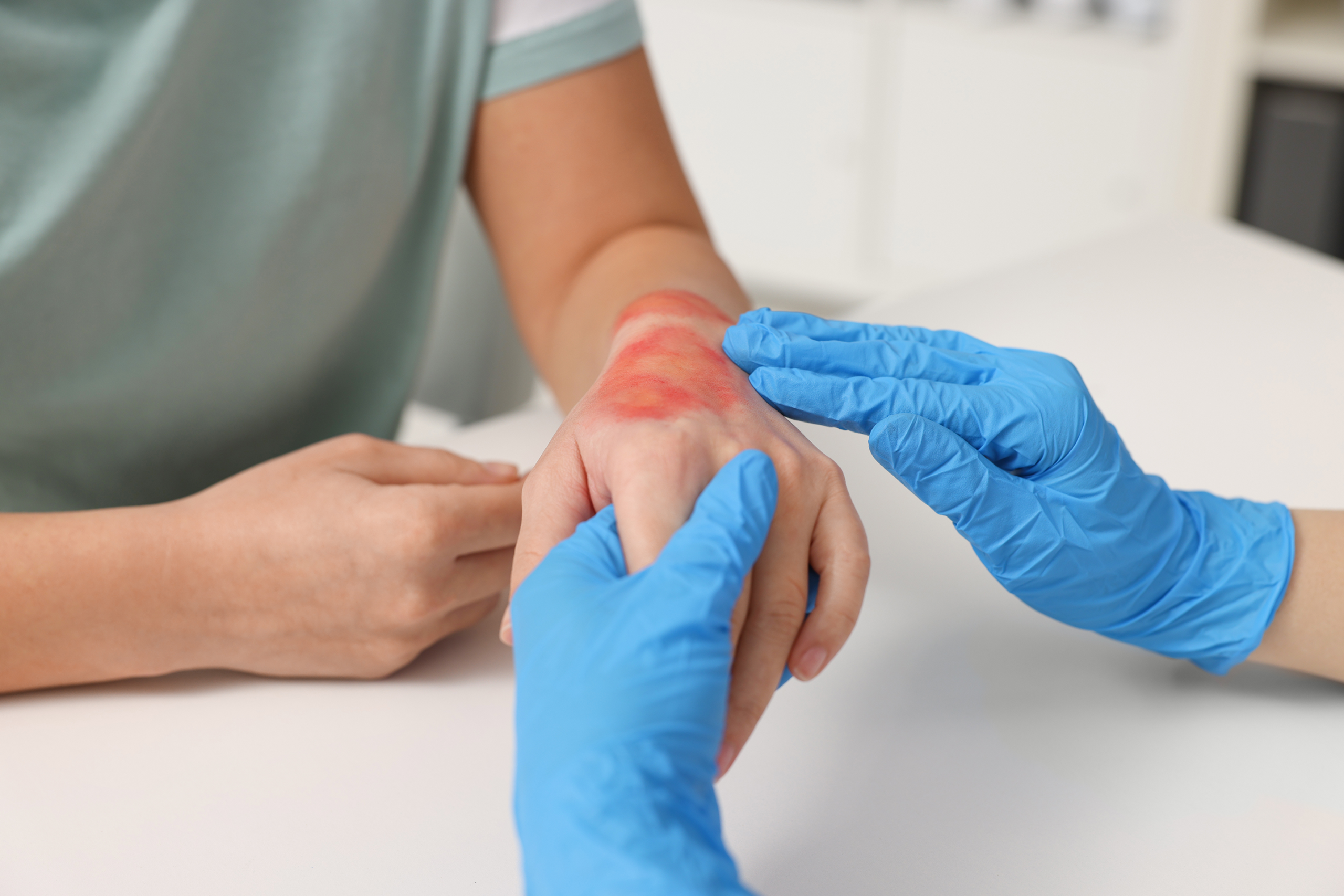
Decubitus ulcers are classified into stages based on the severity of tissue damage, and each stage requires a different treatment approach. Stage 1 is characterized by redness or discoloration that does not fade when pressure is relieved, often accompanied by tenderness. Stage 2 involves partial skin loss, presenting as a blister or shallow open wound. Stage 3 indicates deeper tissue damage that extends into the fat layer, forming a crater-like wound. Stage 4 is the most severe, involving extensive destruction that may reach muscles, tendons, or bones. In some cases, ulcers may be unstageable due to the presence of dead tissue covering the wound, or they may be classified as deep tissue injuries when damage occurs beneath intact skin. Understanding these stages is essential because the effectiveness of decubitus ulcer treatment depends heavily on accurate assessment. Proper staging helps healthcare providers choose the most appropriate interventions and avoid complications.
Importance of Early Diagnosis in Decubitus Ulcer Treatment
Early diagnosis plays a vital role in preventing the progression of pressure ulcers and improving healing outcomes. Detecting the initial signs, such as skin redness, warmth, or swelling, allows for immediate intervention before the condition worsens. Caregivers and healthcare professionals must conduct regular skin inspections, especially for high-risk individuals. Early diagnosis also reduces the likelihood of infection, which can complicate treatment and prolong recovery. Physical assessments are often sufficient, but in some cases, additional diagnostic tools may be used to evaluate the extent of tissue damage. Timely action not only accelerates healing but also minimizes pain and discomfort for the patient. By prioritizing early detection, decubitus ulcer treatment becomes more manageable and less invasive. This proactive approach significantly improves the quality of life for patients dealing with limited mobility.
Core Principles of Decubitus Ulcer Treatment
Effective decubitus ulcer treatment revolves around several core principles that address both the wound and the underlying causes. Pressure relief is the most critical aspect, achieved through frequent repositioning and the use of specialized support surfaces. Maintaining proper hygiene ensures that the wound remains clean and free from harmful bacteria. Enhancing blood circulation is also essential, as it promotes tissue repair and prevents further damage. Addressing underlying medical conditions, such as diabetes or poor nutrition, is equally important in supporting the healing process. A holistic care plan tailored to the patient’s specific needs can significantly improve outcomes. Collaboration between healthcare providers, caregivers, and patients ensures that all aspects of care are addressed. Consistency in applying these principles is key to achieving successful results.
Wound Care Techniques for Effective Healing
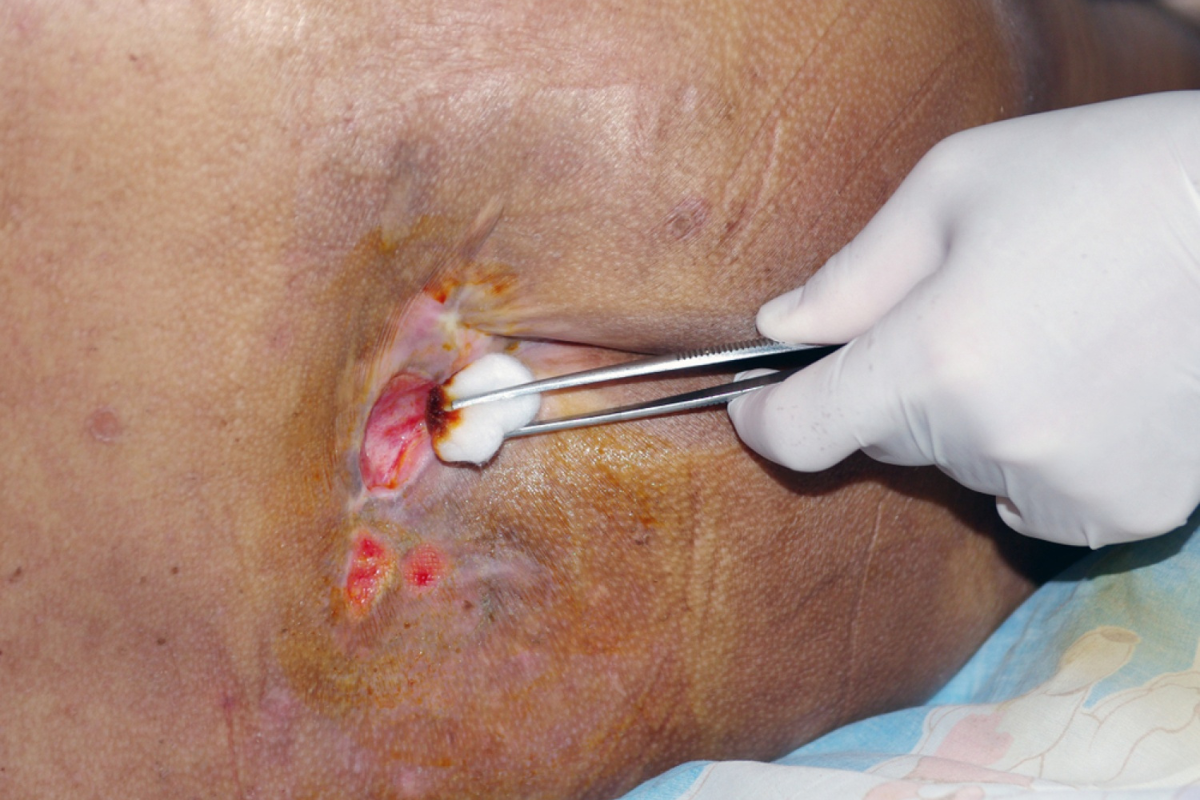
Proper wound care is a cornerstone of successful decubitus ulcer treatment, requiring attention to detail and consistency. Cleaning the wound with gentle solutions helps remove debris and reduce the risk of infection. Dressings play a crucial role in protecting the wound and maintaining a moist environment that promotes healing. Different types of dressings are used depending on the stage and condition of the ulcer. Debridement, or the removal of dead tissue, is often necessary to facilitate the growth of healthy tissue. Infection control measures must be strictly followed to prevent complications that can delay healing. Monitoring the wound regularly allows for adjustments in treatment as needed. A structured wound care routine ensures that the healing process progresses efficiently.
Key Wound Care Practices
- Clean the wound using saline or prescribed solutions
- Apply appropriate dressings based on wound condition
- Change dressings regularly to maintain hygiene
- Remove dead tissue through proper debridement methods
- Watch for signs of infection such as redness or odor
- Keep the surrounding skin dry and protected
- Follow medical guidance for antibiotics if necessary
Advanced Medical Treatments for Severe Cases
For more severe ulcers, advanced medical interventions may be required to support healing. Negative pressure wound therapy is commonly used to remove excess fluid and promote tissue growth. Surgical options, including skin grafts, may be necessary for deep or non-healing wounds. Biologic dressings and growth factors are also used to enhance the body’s natural healing processes. Hyperbaric oxygen therapy can improve oxygen supply to damaged tissues, accelerating recovery. These treatments are typically administered in specialized medical settings under professional supervision. Hospitalization may be required in cases involving severe infection or extensive tissue damage. Advanced treatments are often combined with standard care practices to achieve the best possible outcomes. Choosing the right approach depends on the severity of the ulcer and the patient’s overall health condition.
Role of Nutrition in Decubitus Ulcer Treatment
Nutrition plays a critical role in the healing process, making it an essential component of decubitus ulcer treatment. Protein is vital for tissue repair and regeneration, helping the body rebuild damaged skin. Vitamins such as Vitamin C support collagen production, while minerals like zinc aid in wound healing. Adequate hydration is equally important, as it maintains skin elasticity and prevents dryness. Malnutrition can significantly delay healing and increase the risk of complications. A balanced diet tailored to the patient’s needs can enhance recovery and overall health. In some cases, nutritional supplements may be recommended to address deficiencies. Caregivers should ensure that patients receive proper nourishment to support the healing process. Integrating nutrition into the treatment plan leads to more effective and sustainable results.
Preventive Measures to Avoid Recurrence
Preventing the recurrence of pressure ulcers is just as important as treating existing wounds. Regular repositioning helps distribute pressure evenly and reduces the risk of new ulcers forming. Pressure-relieving mattresses and cushions provide additional support and comfort. Maintaining proper skin hygiene keeps the skin healthy and less prone to damage. Monitoring moisture levels and keeping the skin dry prevents breakdown caused by prolonged exposure to fluids. Educating caregivers and family members ensures that preventive measures are consistently applied. Routine skin inspections allow for early detection of potential issues. Prevention strategies should be incorporated into daily care routines for long-term effectiveness. A proactive approach significantly reduces the likelihood of recurrence.
Home Care vs Professional Medical Treatment
Deciding between home care and professional medical treatment depends on the severity of the ulcer and the patient’s condition. Mild ulcers can often be managed at home with proper guidance and consistent care. However, more advanced stages require professional intervention to prevent complications. Healthcare providers offer specialized expertise and access to advanced treatment options. Signs such as increasing pain, infection, or lack of improvement indicate the need for medical attention. Nurses and wound care specialists play a crucial role in managing complex cases. A multidisciplinary approach ensures comprehensive care that addresses all aspects of the condition. Combining home care with professional support often yields the best results. Making informed decisions about care settings is essential for effective decubitus ulcer treatment.
Emotional and Psychological Impact on Patients
Living with pressure ulcers can take a significant emotional toll on patients, affecting their mental well-being and quality of life. Chronic wounds can lead to feelings of frustration, anxiety, and even depression. The physical discomfort and limitations associated with the condition can further impact a patient’s sense of independence. Emotional support from family members and caregivers is essential in helping patients cope with these challenges. Encouragement and reassurance can boost morale and promote a positive outlook during treatment. Healthcare providers should also consider the psychological aspects of care when developing treatment plans. Addressing emotional needs alongside physical treatment leads to more holistic healing. Creating a supportive environment fosters resilience and improves overall recovery outcomes.
Cost Considerations and Accessibility of Treatment
The cost of decubitus ulcer treatment can vary depending on the severity of the condition and the type of care required. Home-based care is generally more affordable but may not provide the same level of expertise as professional treatment. Hospital care and advanced therapies can be expensive, especially for long-term cases. Insurance coverage and financial assistance programs can help reduce the financial burden on patients and families. Access to affordable treatment options is essential for ensuring consistent care. Balancing cost with quality of care is crucial in achieving effective outcomes. Patients and caregivers should explore all available resources to manage expenses. Planning ahead can make treatment more accessible and sustainable.
FAQ
What is the fastest way to heal a decubitus ulcer
The fastest way involves relieving pressure, maintaining proper wound care, and ensuring good nutrition to support healing.
Can decubitus ulcers be completely cured
Yes, many ulcers can heal completely with proper treatment, especially when addressed early.
How long does decubitus ulcer treatment take
Healing time varies depending on the stage, ranging from a few weeks to several months.
Are home remedies effective for treating pressure ulcers
Some basic care practices can help, but medical guidance is essential for safe and effective treatment.
When should I see a doctor for a bedsore
Seek medical attention if the wound worsens, shows signs of infection, or does not improve with basic care.
What are the best mattresses for preventing pressure ulcers
Pressure-relieving mattresses and cushions designed to distribute weight evenly are highly recommended.
Can decubitus ulcers lead to serious complications
Yes, untreated ulcers can lead to infections, tissue damage, and other serious health issues.
Takeaway
Decubitus ulcer treatment requires a combination of timely intervention, proper wound care, and preventive strategies to ensure successful healing. Addressing the root causes, maintaining consistent care routines, and supporting the patient’s overall health are essential for achieving the best outcomes.