Understanding Severe Wounds and Why Immediate Medical Attention Matters
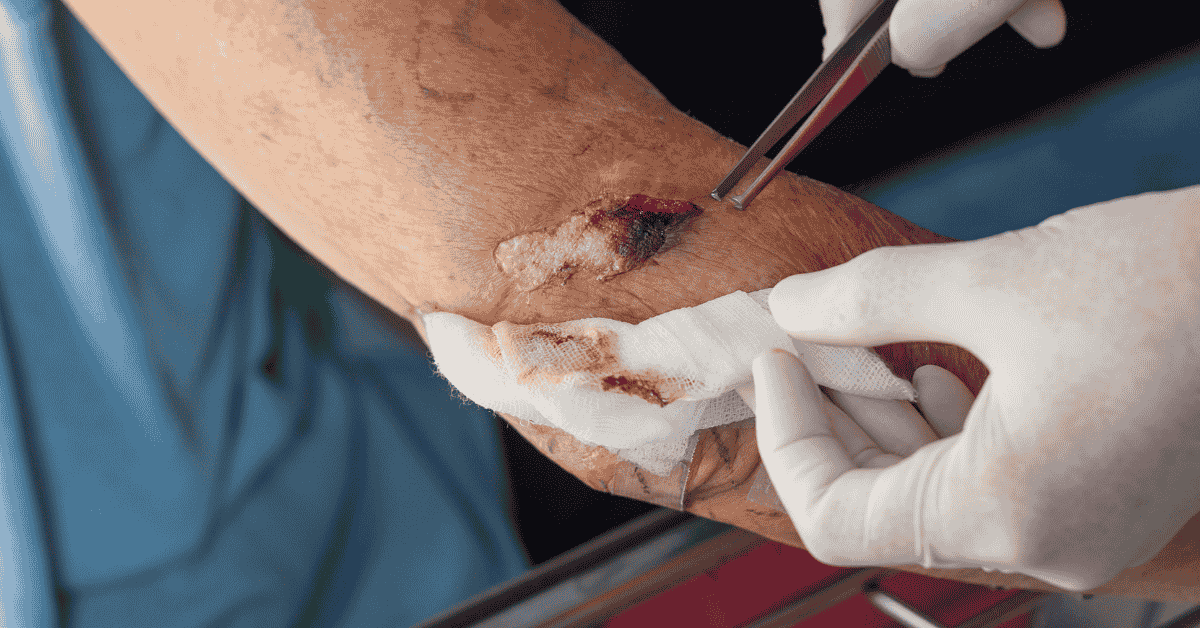
Severe wounds that require sever wound surgery are complex injuries that go beyond the skin surface and often involve deeper structures such as muscles, blood vessels, nerves, or even bones. These injuries commonly occur due to high-impact trauma such as road accidents, workplace incidents, falls from height, or violent physical injuries. Unlike minor cuts or abrasions, severe wounds tend to have significant tissue damage that cannot heal properly without surgical intervention. One of the most critical aspects of managing these injuries is recognizing how quickly complications can develop if treatment is delayed. Excessive bleeding, infection, and tissue death are immediate risks that can worsen within hours. Medical attention is essential not only for survival but also for preserving function and preventing long-term disability. In many cases, sever wound surgery becomes the only viable method to restore structure and stability to the affected area.
Classification of Severe Wounds Requiring Surgery
Severe wounds are categorized based on depth, structure involvement, and contamination level, all of which influence the need for sever wound surgery. Open wounds such as deep lacerations often expose underlying tissues, making them highly susceptible to infection and further damage. Crush injuries are another category where prolonged pressure damages muscles and blood supply, sometimes leading to tissue death. Amputation-level injuries, whether partial or complete, are among the most urgent cases requiring immediate surgical reconstruction. Puncture wounds that penetrate deeply into the body may damage internal organs and require advanced imaging and surgical exploration. Contaminated wounds involving foreign materials such as soil, glass, or metal fragments significantly increase infection risks. Each category demands a different surgical approach depending on severity and location. Proper classification helps medical teams prioritize treatment and determine the urgency of intervention.
Emergency Response Before Sever Wound Surgery
Before a patient undergoes sever wound surgery, emergency response plays a crucial role in stabilizing their condition. The first priority is controlling bleeding using direct pressure or tourniquets when appropriate. Stabilizing the injured area helps prevent further tissue damage and reduces pain. Keeping the wound clean and avoiding contamination is essential, as bacteria can rapidly enter exposed tissue. Emergency responders often elevate the injured limb if possible to reduce blood flow and swelling. It is equally important to monitor the patient’s breathing and consciousness, especially in cases of severe trauma. Immediate transportation to a medical facility ensures that surgical teams can intervene as quickly as possible. Every second counts, as delays can significantly worsen outcomes and increase the complexity of sever wound surgery.
Diagnostic Evaluation Prior to Sever Wound Surgery
Accurate diagnosis is essential before performing sever wound surgery, as it determines the surgical plan and urgency. Physicians begin with a detailed physical examination to assess the extent of visible and hidden damage. Imaging techniques such as X-rays, CT scans, and MRIs help identify fractures, internal bleeding, or foreign objects. Vascular assessments are conducted to determine if blood flow has been compromised, which can threaten limb survival. Neurological testing helps evaluate nerve damage that may affect sensation or movement. Laboratory tests are also performed to check for infection or blood loss severity. In unstable patients, rapid diagnostic tools are prioritized to avoid delays in treatment. These evaluations allow surgeons to plan a precise and effective approach to sever wound surgery.
Surgical Techniques Used in Sever Wound Surgery
The process of sever wound surgery involves multiple advanced techniques designed to repair and restore damaged tissues. One of the first steps is debridement, which involves removing dead or contaminated tissue to prevent infection. Surgeons then focus on controlling bleeding using specialized hemostatic methods. Depending on the injury, wounds may be closed immediately or left open for delayed closure to reduce infection risk. Skin grafting is often used when large areas of skin are lost, helping restore coverage and protection. Microsurgery may be required to repair damaged nerves and blood vessels with precision. In some cases, surgical staples or sutures are used to hold tissues together during healing. Vacuum-assisted closure systems may also be applied to promote faster healing by improving blood flow and reducing fluid buildup.
Role of Reconstructive Surgery in Severe Wound Management
Reconstructive procedures are often a critical part of sever wound surgery, especially when large portions of tissue are lost. The goal of reconstructive surgery is not only to close the wound but also to restore function and appearance. Surgeons may use tissue from other parts of the body to rebuild damaged areas. Bone reconstruction may be necessary when fractures are severe or complex. In extreme cases, prosthetic integration is considered when natural reconstruction is not possible. Skin expansion techniques can help grow additional tissue for large wound coverage. The process is highly individualized depending on the location and severity of the injury. Reconstructive efforts significantly improve mobility, appearance, and long-term quality of life.
Infection Control During and After Sever Wound Surgery
Infection prevention is a major focus in sever wound surgery due to the high risk associated with open injuries. Surgical environments are maintained under strict sterile conditions to reduce bacterial exposure. Antibiotics are often administered before and after surgery to prevent infection development. Surgeons carefully monitor wounds for signs of redness, swelling, or unusual discharge. Proper dressing techniques help maintain a clean environment for healing tissues. Contaminated wounds require more aggressive cleaning and debridement procedures. In severe cases, infections can spread into the bloodstream, leading to life-threatening complications. Continuous monitoring ensures that any signs of infection are addressed immediately.
Pain Management Strategies in Severe Wound Surgery Patients
Pain control is an essential aspect of sever wound surgery, both during and after the procedure. Anesthesia options include local, regional, or general anesthesia depending on injury severity. During surgery, patients are carefully monitored to ensure they remain stable and pain-free. After surgery, medications are prescribed to manage discomfort and inflammation. Nerve blocks may be used for targeted pain relief in specific areas. Multimodal pain management strategies combine different medications to improve effectiveness while reducing side effects. Psychological support is also important, as trauma-related pain can have emotional impacts. Proper pain control helps improve recovery outcomes and patient comfort.
Post-Surgical Recovery and Healing Process
Recovery after sever wound surgery involves multiple stages of healing that occur over weeks or months. Initially, the body focuses on stopping bleeding and preventing infection. Inflammatory responses help clear damaged tissue and begin repair processes. New tissue formation gradually replaces injured areas during the healing phase. Physical therapy is often required to restore strength and mobility. Scar tissue formation is monitored to ensure it does not restrict movement. Nutrition plays a key role in supporting tissue regeneration and overall recovery. Regular follow-up appointments help track progress and detect any complications early.
Potential Complications of Sever Wound Surgery
Although sever wound surgery is highly effective, complications can still occur depending on injury severity. Excessive bleeding may occur during or after surgery, requiring additional intervention. Infections remain one of the most common risks, especially in contaminated wounds. Some patients may experience delayed healing due to underlying health conditions. Nerve damage can result in reduced sensation or mobility in affected areas. Scar tissue may form excessively, leading to stiffness or discomfort. In rare cases, grafts or repairs may fail and require revision surgery. Continuous medical monitoring helps reduce the likelihood of these complications.
Advances in Sever Wound Surgery Techniques and Technology
Modern medicine has significantly improved outcomes in sever wound surgery through technological advancements. Robotic-assisted surgery allows for greater precision in delicate procedures. Regenerative medicine is being explored to enhance tissue repair and growth. 3D-printed scaffolds are used to support new tissue development in complex injuries. Bioengineered skin substitutes offer alternatives for patients with extensive skin loss. Smart wound dressings can monitor healing conditions in real time. Minimally invasive techniques reduce recovery time and surgical trauma. These innovations continue to improve survival rates and functional recovery.
Rehabilitation and Long-Term Care After Severe Wound Surgery
Rehabilitation is an essential part of recovery after sever wound surgery, focusing on restoring independence and mobility. Physical therapy helps patients regain strength and coordination in affected areas. Occupational therapy supports the return to daily activities and work functions. Emotional and psychological counseling may be necessary to address trauma-related stress. Long-term care includes monitoring for chronic pain or mobility limitations. Patients may need adaptive devices depending on the severity of their injuries. Lifestyle adjustments can help prevent further complications and support healing. Ongoing support systems play a critical role in long-term recovery success.
When to Seek Specialized Care for Severe Wounds
Specialized care becomes necessary when injuries are beyond the scope of basic medical treatment and require sever wound surgery. Signs such as uncontrolled bleeding, deep tissue exposure, or loss of sensation indicate urgent medical attention. Severe swelling or deformity may suggest internal damage requiring surgical evaluation. If infection symptoms appear, immediate treatment is essential to prevent complications. Trauma centers are equipped with specialized teams for complex wound management. Delayed symptoms such as persistent pain or limited movement should not be ignored. Early intervention significantly improves outcomes and reduces long-term damage.
Prevention Strategies to Reduce Risk of Severe Wounds
Preventing injuries that require sever wound surgery involves adopting safety measures in daily life. Workplace safety protocols help reduce risks in high-hazard environments. Wearing protective equipment during sports or industrial work is essential. Road safety practices, including seatbelt use and cautious driving, reduce accident-related injuries. Home safety awareness can prevent falls and accidental injuries. Education programs help individuals understand risk factors and prevention techniques. Regular safety training in workplaces further minimizes injury risks. Prevention remains the most effective strategy for avoiding severe trauma.
Frequently Asked Questions (FAQ)
What is sever wound surgery used for?
It is used to treat deep, complex injuries involving muscles, nerves, blood vessels, or bones that cannot heal without surgical intervention.
How long does recovery take after sever wound surgery?
Recovery time varies depending on injury severity, ranging from weeks to several months.
Is sever wound surgery always urgent?
Many cases are emergencies, especially when there is heavy bleeding or tissue damage.
Can severe wounds heal without surgery?
Some minor severe wounds may heal with medical care, but most deep injuries require surgery.
What are the risks involved?
Risks include infection, bleeding, nerve damage, and delayed healing.
Will scarring occur after surgery?
Yes, but reconstructive techniques aim to minimize visible scarring and improve function.
Is physical therapy required?
In most cases, yes, to restore movement and strength.
Key Insight Section
Effective management of sever wound surgery depends on rapid response, precise surgical techniques, and structured recovery planning. Early intervention dramatically improves patient outcomes and reduces long-term complications.